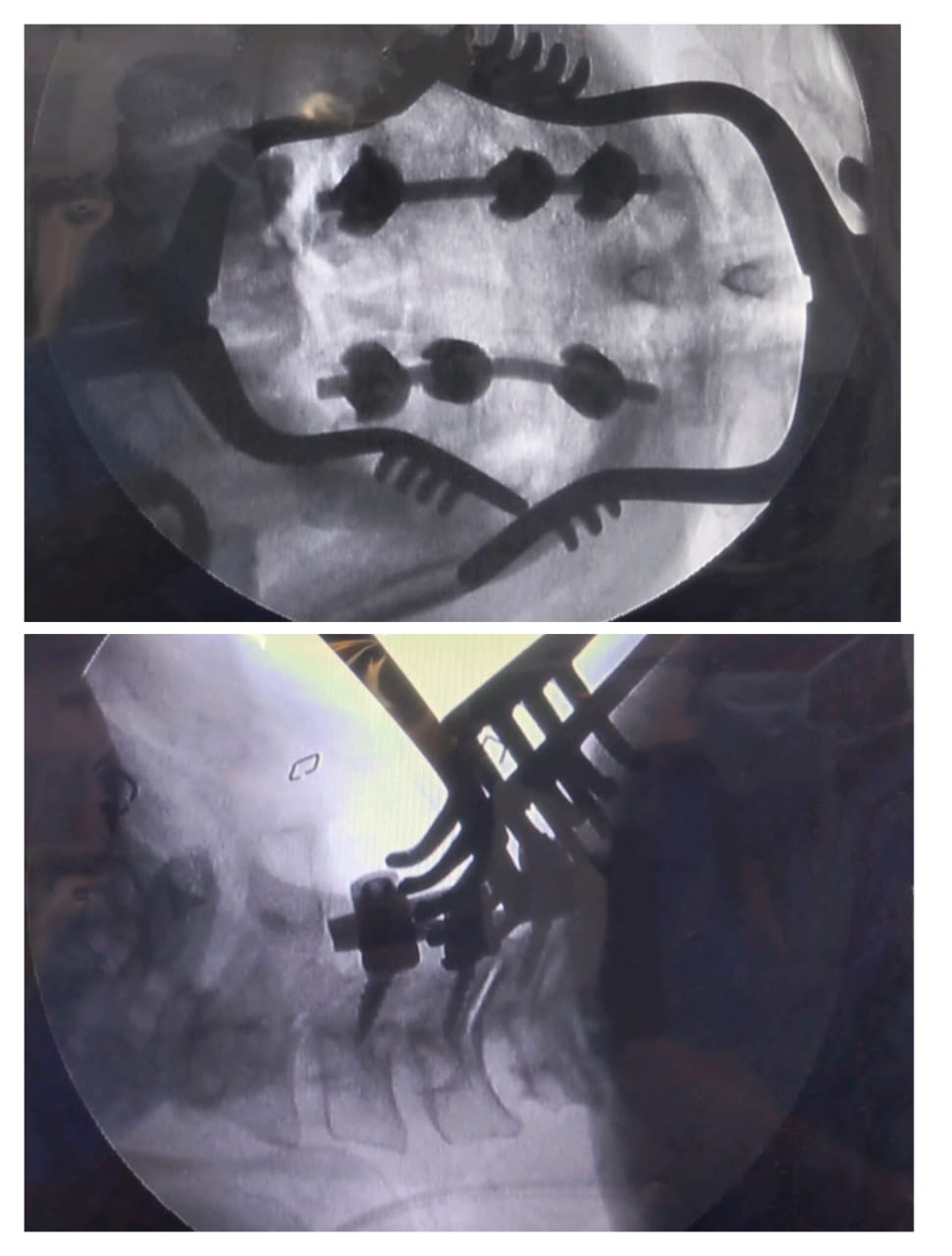
Case Study 1: Cervical Spondylosis
A male patient, aged 60 years, presented to us with a complaint of severe neck pain and difficulty in lifting objects with his hands. He was also experiencing difficulty in opening and closing the buttons of his shirts. After conducting an MRI of the cervical spine, we diagnosed him with cervical spondylotic myelopathy. The patient was given satisfactory counselling and underwent a successful operation. Currently, his pain has been alleviated by 80-90%, and he is now able to open and close the buttons of his shirts. Furthermore, his hand grip has improved by 50%.
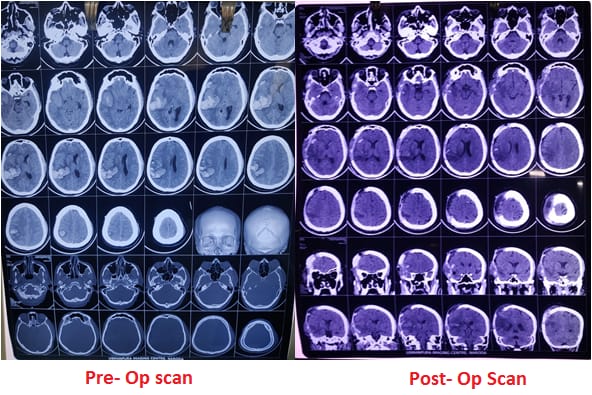
Case Study 2: Temporo-parietal Hematoma
A male patient who was 40 years old arrived with an RTA injury and suffered a temporo-parietal hematoma, as revealed by a CT scan of his head. We counseled the patient's relative on the need for urgent surgery to remove the hematoma and, once consent was given, performed the operation. The postoperative CT scan showed that almost all of the hematoma had been removed, and the patient made a good recovery, leading to his discharge from the hospital.

Case Study 3: Herniated Disc
A male patient, aged 35, presented to our clinic with a primary concern of intense lower back pain that was also radiating to his left lower limb. The patient was experiencing such severe discomfort that he was unable to walk or stand. After performing surgery to remove the herniated disc, the patient experienced immediate relief and was able to move about without difficulty on the following day.
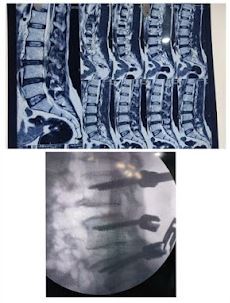
Case Study 4: Complain of Sever Back Pain
A male patient, aged 50, presented to our facility with a complaint of severe back pain that radiated to both lower limbs. We provided the patient with an explanation about the surgical procedure, and subsequently performed the operation. Currently, the patient is able to carry out all of his tasks without experiencing any pain.
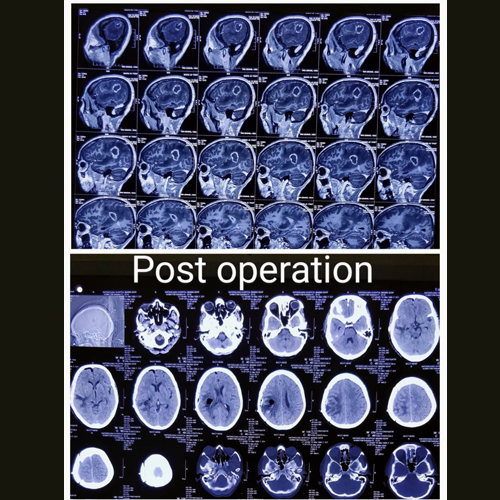
Case Study 5: Successful Surgical Treatment of Right Temporoparietal Brain Tumor Leading to Hemiparesis Recovery
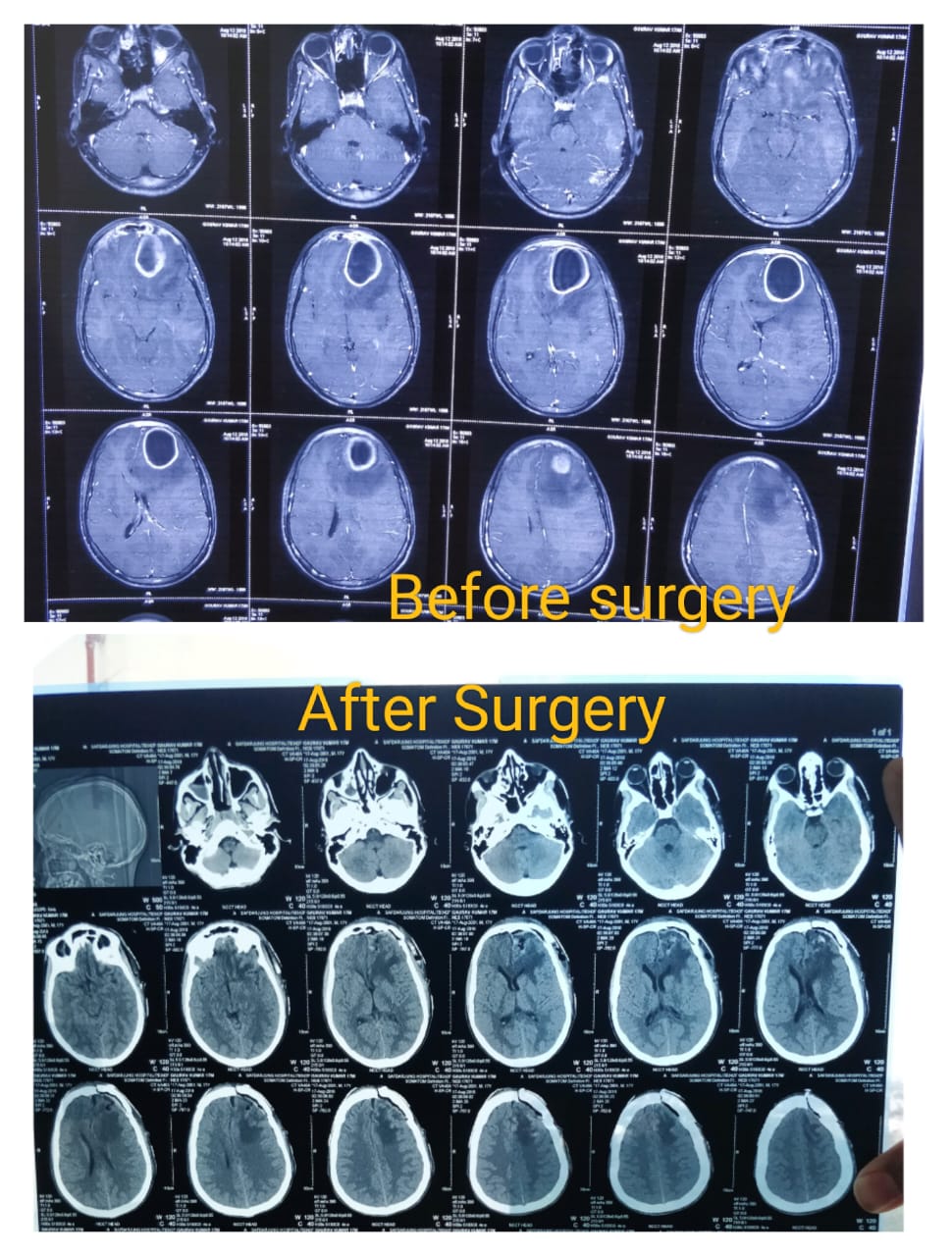
This case study presents the successful surgical treatment of a 52-year-old female patient with left side hemiparesis caused by a right temporoparietal brain tumor. The patient underwent surgical intervention, resulting in nearly complete removal of the tumor. Subsequently, with the aid of physiotherapy, the patient experienced a remarkable recovery from her hemiparesis within a period of two months. This case highlights the importance of early diagnosis, prompt surgical intervention, and comprehensive post-operative care in achieving positive outcomes for patients with brain tumors leading to neurological deficits.
This case study emphasizes the importance of a multidisciplinary approach in managing such cases and highlights the potential for functional recovery even in severe neurological deficits caused by brain tumors.

Case Study 6: Successful Emergency Surgery for Traumatic Brain Injury Resulting from a Road Traffic Accident
This case study presents the successful management of a 15-year-old male patient who presented in an unconscious state following a road traffic accident. The patient underwent emergency surgery to address the traumatic brain injury. Following the procedure, the patient made a remarkable recovery, regained consciousness, and exhibited no neurological deficits upon discharge. This case highlights the importance of prompt surgical intervention in improving outcomes for patients with severe traumatic brain injuries.
This case study emphasizes the importance of prompt diagnosis, effective communication with the patient's family, and expedited surgical intervention in optimizing outcomes for young individuals with TBI.
Case Study 7: Successful Surgical Treatment of Frontal Abscess in a 17-Year-Old Male Patient with Recurrent Sinusitis
This case study presents the successful surgical management of a frontal abscess in a 17-year-old male patient with a history of severe headaches, vomiting, and recurrent sinusitis.
The patient underwent an MRI, which revealed the presence of a frontal abscess. The operative process promptly performed a surgical excision of the abscess, leading to a complete resolution of symptoms. The patient was discharged without any neurological deficits.
This case highlights the importance of early diagnosis, timely intervention, and comprehensive management in patients with intracranial abscesses.
Brain & Spine related problems & FAQs
-
What is Cervical Spondylosis?
Cervical spondylosis, also known as cervical osteoarthritis, is a condition that affects the joints, bones, and discs in the neck region. It is a degenerative condition that commonly occurs in older adults and can cause pain and stiffness in the neck, shoulders, and upper back.
Cervical spondylosis is caused by wear and tear on the cervical spine, which can lead to the breakdown of the spinal discs and the formation of bone spurs. The condition can also cause the narrowing of the spinal canal, which can put pressure on the spinal cord and nerve roots.
Common symptoms of cervical spondylosis include neck pain and stiffness, headaches, dizziness, tingling or numbness in the arms and hands, and weakness in the arms or legs. Treatment options include medication, physical therapy, and surgery in severe cases.
-
What is the main cause of Cervical Spondylosis?
Cervical spondylosis is a degenerative condition that affects the cervical spine (neck region) and is primarily caused by age-related wear and tear of the bones, discs, and ligaments in the neck. As we age, the discs in our spine lose their elasticity and cushioning ability, which can lead to a narrowing of the spaces between the vertebrae (the bones that make up the spine) and the development of bone spurs. These changes can put pressure on the spinal cord and nerves that run through the neck, leading to symptoms such as neck pain, stiffness, and tingling or numbness in the arms and hands. Other risk factors for cervical spondylosis include a history of neck injuries or trauma, poor posture, and genetic factors.
-
What is Temporo-parietal Hematoma?
A temporoparietal hematoma refers to bleeding that occurs in the area of the brain where the temporal and parietal lobes meet. These lobes are located on the sides and top of the brain, respectively. Hematomas occur when there is bleeding inside the brain, usually as a result of trauma, a ruptured blood vessel, or a clotting disorder.
Symptoms of a temporoparietal hematoma can include headache, nausea, vomiting, confusion, weakness, seizures, and loss of consciousness. Treatment depends on the severity of the bleeding and the patient's overall health. In some cases, surgery may be necessary to remove the hematoma and relieve pressure on the brain. Recovery from a temporoparietal hematoma can be a lengthy process and may involve rehabilitation and physical therapy.
-
What is Herniated Disc?
A herniated disc, also known as a slipped or ruptured disc, is a condition that occurs when the soft inner core of a spinal disc pushes through a tear in the outer layer of the disc. The spinal discs are located between the vertebrae of the spine and act as shock absorbers, allowing for movement and flexibility.
When a disc herniates, it can put pressure on the spinal nerves or spinal cord, causing pain, weakness, numbness, or tingling in the arms or legs, depending on the location of the affected disc. Herniated discs can occur in any part of the spine, but they are most common in the lower back (lumbar spine) and neck (cervical spine).
Herniated discs can be caused by degenerative changes in the spine due to aging, as well as trauma or injury to the spine. Treatment options for herniated discs include rest, physical therapy, medications, and in some cases, surgery.
